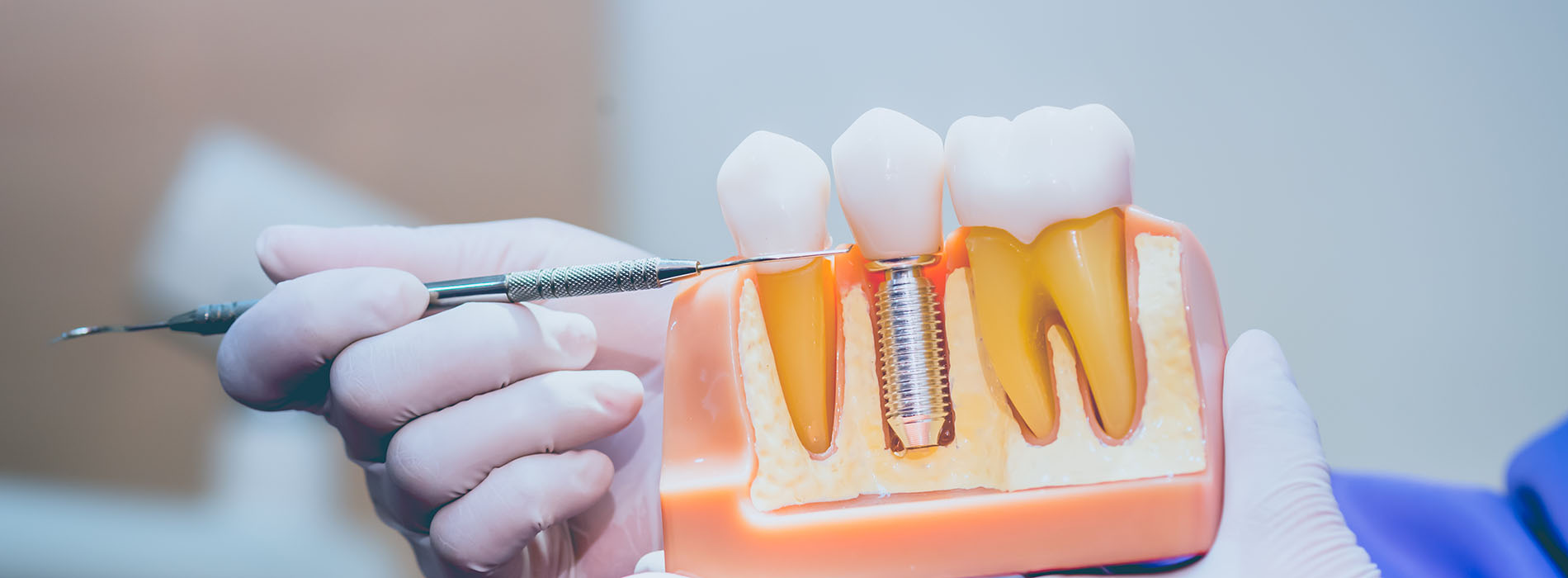
Missing teeth can change how you look, how you eat, and even how you feel about everyday interactions. Implant restorations are designed to replace lost teeth in a way that restores natural function while preserving the facial structure beneath the gumline. Rather than masking a gap, modern implant restorations rebuild the connection between tooth and jaw so patients can speak, chew, and smile with confidence.
Unlike some removable options, implant restorations are anchored to titanium or zirconia implants that integrate with bone. This stable foundation supports crowns, bridges, or hybrid prostheses and resists the slipping or shifting that can come with traditional dentures. The result is a solution that behaves much like a natural tooth—reliable, discreet, and built to last when cared for properly.
At Strohman Family Dental, we approach each restoration with an eye toward long-term function and appearance. That begins with understanding a patient’s goals, oral health history, and the specific anatomy of their mouth. Thoughtful planning helps ensure the restoration looks natural and performs well in day-to-day life.
When planned and executed carefully, implant restorations can protect surrounding teeth and the jawbone itself. By replacing the tooth root’s role, implants help preserve bone density and maintain the contours of the smile—benefits that extend well beyond cosmetic improvement.
Implant success depends on a biological process called osseointegration, where bone cells grow tightly around the implant surface. This creates a strong mechanical and biological bond that allows the implant to support chewing forces much like a natural root. Contemporary implant materials and surface designs are engineered to encourage this integration while minimizing complications.
Before placing an implant, we evaluate bone volume and quality using digital imaging. If the jaw lacks sufficient bone, there are predictable grafting techniques that can rebuild the foundation. These preparatory steps ensure the implant has the best possible environment for long-term stability.
After placement, a healing period allows the bone to mature around the implant. During this time, temporary restorations can preserve aesthetics and function while protecting the surgical site. Once integration is complete, the implant becomes ready to carry a final restoration—carefully matched in shape, color, and bite to the patient’s natural teeth.
Worldwide clinical experience shows that with proper planning and maintenance, integrated implants provide a durable base for replacement teeth. The aim is always to recreate the balance between strength, comfort, and a natural appearance.
Creating an implant restoration that blends seamlessly with the rest of the smile involves more than matching tooth color. Our technicians consider tooth shape, translucency, and how light reflects off the surface to produce lifelike results. For multi-tooth replacements, harmony among adjacent restorations is essential so the smile reads as uniform and natural.
Material choices matter. Ceramic crowns and bridges offer excellent aesthetics and biocompatibility, while screw-retained and cement-retained options each have advantages depending on access and soft-tissue considerations. The right selection is based on the clinical situation and the patient’s long-term goals rather than a one-size-fits-all approach.
Digital workflows—such as intraoral scanning and CAD/CAM milling—allow for precise communication between the dental team and the lab. This reduces guesswork and helps deliver restorations that fit accurately and require fewer adjustments. When margin fit and occlusion are optimized, patients enjoy a more comfortable final restoration from day one.
Soft-tissue management around the implant is another important design element. Properly contoured gingival architecture keeps the restoration looking natural at the gumline and supports lasting oral health. Attention to these details makes the difference between a restoration that simply works and one that truly feels like your own tooth.
An effective implant restoration starts with a comprehensive plan. The process begins with a thorough exam, including digital radiographs and discussion of medical history. From there, we map out the steps—whether it’s a single crown, a multi-tooth bridge, or an implant-supported denture—so patients understand the timeline and what each phase involves.
Placement typically requires a minor surgical procedure performed with sterile technique and appropriate anesthesia for comfort. Many patients describe the experience as straightforward, and our team provides clear post-operative instructions to support healing. Follow-up visits during the integration phase allow us to monitor progress and address any questions promptly.
Once the implant has integrated, impressions or digital scans are taken for the final restoration. This is where fit, occlusion, and aesthetics are refined. A try-in may be performed to ensure color and form meet expectations before the restoration is permanently seated. The finished result restores chewing efficiency and improves overall oral balance.
Long-term success hinges on routine care and sensible habits. Daily oral hygiene—brushing thoroughly, cleaning around implants with interdental brushes or floss designed for implants, and maintaining a clean oral environment—helps prevent inflammation of the surrounding tissues. Regular professional check-ups allow early detection of issues that could compromise the restoration.
Behavioral factors also play a role: avoiding excessive forces like chewing ice or using teeth as tools reduces the chance of mechanical complications. For patients who grind or clench, protective appliances can limit harmful pressure and extend the life of restorations. Our team evaluates risk factors and recommends appropriate measures to protect your investment in oral health.
When issues do arise, such as loosening of a crown or irritation around the gumline, prompt attention increases the likelihood of a straightforward resolution. Routine maintenance visits include assessments of the implant, the prosthetic components, and the supporting tissues so any concerns are caught early and managed conservatively.
Implant restorations offer a reliable path to restoring function and appearance while protecting the long-term health of the jaw. If you’d like to learn more about how implant-supported crowns or bridges might fit into your treatment plan, the team at Strohman Family Dental is available to discuss options and next steps. Contact us for more information or to arrange a consultation.
Implant restorations are replacement teeth that attach to dental implants, which act as artificial tooth roots anchored in the jawbone. Unlike removable dentures or traditional bridges that rely on neighboring teeth or suction, implant restorations are supported by the bone through the implant, providing greater stability for chewing and speaking. They can support single crowns, multi-tooth bridges, or full-arch prostheses depending on the clinical need.
The design of an implant restoration focuses on recreating form and function while preserving surrounding tissues. Because the implant replaces the root, it helps maintain bone volume and facial contours that can be lost after tooth extraction. This structural benefit distinguishes implant restorations from solutions that only replace visible tooth structure.
Osseointegration is the biological process in which bone cells attach directly to the implant surface, forming a stable and lasting connection. This bond creates a mechanical foundation capable of transmitting chewing forces into the jawbone much like a natural tooth root, which supports durable prosthetic function. Modern implant materials and surface treatments are engineered to encourage predictable osseointegration while minimizing complications.
Successful osseointegration depends on bone quality, precise surgical technique, and an appropriate healing period after placement. Digital imaging and careful planning help ensure implants are positioned to maximize bone contact and load distribution. When integration is complete, the restored tooth can provide reliable function and comfort over many years with proper care.
A good candidate for implant restorations has adequate jawbone volume and healthy oral tissues, along with a commitment to maintaining regular oral hygiene and dental visits. Overall medical health is also considered, since systemic conditions and certain medications can affect healing and implant success. During the evaluation we review medical history, oral health, and imaging to determine whether implants are appropriate.
For patients with insufficient bone or complex anatomy, predictable preparatory procedures such as bone grafting or ridge augmentation can expand candidacy by rebuilding a suitable foundation. Smoking cessation and management of conditions like uncontrolled diabetes are additional measures that improve outcomes. Our team at Strohman Family Dental works with patients to identify solutions and create individualized treatment plans that align with their goals.
The treatment process begins with a comprehensive exam that includes digital radiographs or CBCT imaging and a review of medical and dental history. Planning establishes the number and position of implants, any need for grafting, and the type of final prosthesis, whether a crown, bridge, or hybrid denture. This phase ensures the surgical and restorative steps are coordinated for predictable results.
Placement of the implant is a minor surgical procedure performed under local anesthesia and, if needed, additional sedation for comfort. After placement a healing interval allows osseointegration to occur, typically several months depending on bone quality and the clinical situation. Once integration is confirmed, impressions or digital scans are taken and the final restoration is fabricated, fitted, and adjusted for optimal form and function.
If the jaw lacks sufficient bone volume to support an implant, there are established grafting techniques that can rebuild the foundation prior to or at the time of implant placement. Options include bone grafts using autogenous, allograft, or synthetic bone substitutes as well as guided bone regeneration with barrier membranes. The choice of technique depends on the size and location of the defect, the desired amount of augmentation, and the patient’s overall health.
In some cases, procedures such as sinus lifts or ridge expansion are required to create the necessary height or width of bone. These preparatory surgeries are predictable and allow implants to be placed in a stable, well-supported position once healing is complete. Careful planning with digital imaging helps determine the most appropriate sequence to achieve long-term implant success.
Implant fixtures are commonly made from titanium or zirconia because of their biocompatibility and strength, while the visible restorations are often crafted from high-quality ceramics. Ceramic crowns and bridges provide lifelike translucency and color matching, and they are well suited for front and back teeth depending on functional demands. Material selection balances aesthetics, durability, and the clinical environment around the implant.
Retention methods for restorations include screw-retained and cement-retained designs, each with distinct advantages related to retrievability and soft-tissue management. The restorative team evaluates factors such as access, occlusion, hygiene ability, and soft-tissue contours when selecting materials and retention. Digital workflows and CAD/CAM fabrication further enhance fit and consistency across the restorative process.
Daily oral hygiene is essential for maintaining implant health and preventing inflammation of the surrounding tissues, known as peri-implant mucositis or peri-implantitis. Patients should brush thoroughly, clean under and around prosthetic components with interdental brushes or floss designed for implants, and follow any specific home-care instructions provided by the dental team. Good oral hygiene reduces bacterial buildup and supports the longevity of both the implant and the restoration.
Regular professional maintenance visits are equally important so the clinician can assess tissue health, prosthetic fit, and occlusion, and perform professional cleaning as needed. For patients who grind their teeth or place excessive forces on restorations, nightguards or occlusal adjustments can protect the implant prosthesis. Prompt attention to any loosening, discomfort, or changes in gum appearance increases the likelihood of a conservative resolution.
Complications can include soft-tissue inflammation, peri-implant bone loss, prosthetic loosening or fracture, and, less commonly, implant failure. Many issues are related to bacterial accumulation, occlusal overload, or systemic factors that affect healing, and early detection is critical for favorable outcomes. Regular monitoring and maintenance help identify problems before they progress and often allow for minimally invasive management.
Treatment may involve professional debridement, antimicrobial therapy, adjustment of prosthetic components, occlusal equilibration, or surgical intervention in cases of advanced bone loss. The clinical team assesses the specific cause and tailors the response to preserve the implant and surrounding tissues whenever possible. Clear communication and timely follow-up are important parts of effective complication management.
Implant-supported dentures and bridges are anchored to implants in the jaw, which provides increased stability and chewing efficiency compared with traditional removable dentures that rely on soft-tissue support. Fixed implant bridges replace multiple adjacent teeth without altering neighboring healthy teeth as a traditional fixed bridge often does, because implants carry the load instead of natural tooth structure. These differences can improve comfort, speech, and confidence in daily function.
The implant-supported approach also helps preserve jawbone by transmitting functional forces into the bone, whereas traditional dentures may accelerate bone loss over time due to lack of root stimulation. Choosing between implant-supported and conventional options depends on the patient’s anatomy, oral-health priorities, and long-term goals, and it is determined during the comprehensive planning process.
To explore implant restorations, schedule a consultation that includes a thorough clinical exam and appropriate digital imaging so the dental team can evaluate bone volume, occlusion, and overall oral-health needs. During the visit you can discuss treatment options, anticipated steps in the care plan, and any preparatory procedures that may be required. The consultation is an opportunity to review medical history, expectations for function and appearance, and practical aspects of the timeline.
To arrange an appointment, contact Strohman Family Dental at (515) 295-5200 or visit the office at 301 E Call Street in Algona, AI 50511. Our team will gather necessary records, coordinate imaging if needed, and outline the next steps to determine candidacy for implant restorations. A clear, planned approach helps ensure that the chosen solution meets both functional and aesthetic goals.


