
At the office of Strohman Family Dental, our priority is protecting your long-term oral health while minimizing discomfort and anxiety. We begin every treatment discussion by exploring conservative options to preserve natural tooth structure. Extraction is considered only when those options are exhausted or when removing a tooth is the safest path forward for the mouth as a whole.
Understanding why an extraction is recommended helps patients feel more in control. We take time to review your dental and medical history, explain the reason for removal in plain language, and outline the steps we’ll take to make the experience predictable and comfortable. You’ll always know what to expect before any procedure begins.
Our team focuses on combining clinical experience with modern tools and careful planning. This approach helps us limit complications, support smooth healing, and coordinate next steps for restoring function and appearance when a replacement is needed.
Stubborn or over-retained baby (deciduous) teeth
Sometimes a primary tooth does not loosen on schedule because its roots fail to resorb or the tooth becomes fused to the bone. When this interferes with the eruption or alignment of the permanent tooth beneath it, removing the baby tooth can prevent crowding and orthodontic complications later on.
Permanent teeth that are too damaged to restore
Decay that penetrates deep into a tooth can destroy structural support and reach the nerve. When there is insufficient healthy tooth left to support a restoration, extraction may be the safest option to prevent ongoing infection and protect neighboring teeth.
Severe fractures or cracks that compromise the tooth
Teeth can sustain complex fractures that affect their roots or split them in ways that can’t be predictably repaired. In those cases, removal eliminates a source of pain and infection and allows us to discuss replacement plans that restore chewing ability and aesthetics.
Advanced periodontal (gum) disease
When periodontal disease has destroyed the supporting bone and connective tissues around a tooth, that tooth can become loose and painful. Removing such a tooth can improve overall oral health and make it easier to treat the remaining dentition.
Wisdom teeth that are impacted or causing harm
Third molars often lack adequate space to erupt properly. They may become impacted, develop decay, or push on neighboring teeth. We recommend removal when these teeth threaten comfort, alignment, or oral hygiene.
Extractions as part of orthodontic planning
When the dental arch lacks sufficient room for all permanent teeth, selective extraction can create space to align teeth predictably. Any decision of this nature is coordinated closely with your orthodontic provider to achieve the best functional and aesthetic result.
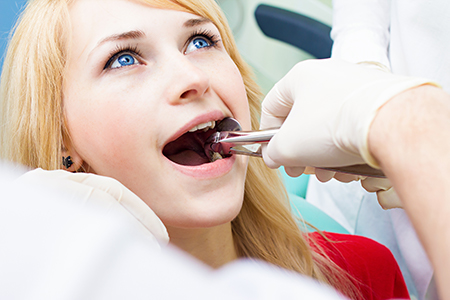
Before any procedure, we perform a careful evaluation that typically includes a clinical exam and digital radiographs to visualize roots and surrounding bone. We review medications, medical conditions, and any special considerations so we can tailor the treatment plan and take appropriate precautions. If necessary, we will seek medical clearance from your physician.
Communication about anesthesia and comfort is central to our approach. Most extractions are performed under local anesthesia, which numbs the area completely. For patients who prefer additional relaxation, we discuss sedation options and the benefits and requirements of each so you can make an informed choice.
Our objective is to keep the procedure efficient and gentle. We’ll explain each step in advance, from how the area will be numbed to what you can expect immediately after the tooth is removed. Clear instructions and calm guidance help reduce anxiety and create a smoother experience.
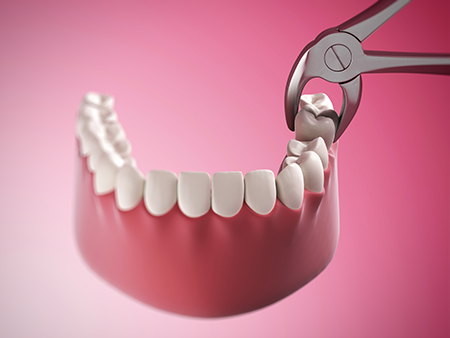
Exodontia falls into two main categories, and the type of procedure determines the technique and recovery considerations:
Simple extractions are used when the tooth is visible in the mouth and the root anatomy is straightforward. After numbing the area, the dentist loosens the tooth and removes it with controlled force using appropriate instruments. The process is typically quick, and patients are monitored until they are comfortable and stable before leaving the office.
Surgical extractions are required when a tooth is broken at the gum line, fused to the bone, or impacted below the gum. These procedures may involve a small incision in the gum and removal of a bit of bone to access the tooth. In cases that are more complex, we may refer to or collaborate with an oral and maxillofacial surgeon to ensure the safest outcome.
Healing after an extraction is a process we plan for in advance. Every patient receives customized post-operative guidance that covers medication use, activity limits, diet, and follow-up care. Most people experience some swelling and mild discomfort, both of which are temporary and manageable when instructions are followed.
We emphasize practical measures that support healing, protect the blood clot in the socket, and reduce the chance of complications. If you have other health concerns or take medications that affect healing, we coordinate with your medical team to optimize recovery.
Keeping the surgical site protected and observing changes in pain, swelling, or bleeding are key. Any unexpected symptoms—such as persistent heavy bleeding, increasing pain after the first few days, or signs of infection—should prompt contact with our office so we can intervene promptly.
Apply gauze to control bleeding
We place gauze over the extraction site to encourage clot formation. Bite gently and keep pressure in place as instructed; you can change the gauze after the first hour if needed. Some light oozing for a day or so is common, but persistent heavy bleeding should be reported.
Protect numb tissues
While the anesthetic is still active, avoid chewing or touching the area. Lips, cheeks, and tongue can be inadvertently bitten while numb, so take care until normal sensation returns.
Follow medication directions carefully
Antibiotics:
If antibiotics are prescribed, take them exactly as directed and complete the full course to reduce infection risk.
Pain control:
Start pain medication before the numbness fully wears off when recommended, and use over-the-counter options as advised for mild discomfort. Use prescription analgesics only as prescribed.
Allow the clot to form
Avoid rinsing vigorously, spitting, sucking through a straw, or other actions that could dislodge the blood clot for the first 24–48 hours; protecting the clot is essential for uncomplicated healing.
Manage swelling
Apply ice to the face over the extraction area during short intervals on the first day to reduce swelling. Follow the schedule we recommend for best results.
Avoid smoking
Tobacco products impede clot formation and slow healing. Refrain from smoking for at least a week after the extraction to reduce complications.
Stick to gentle foods
Choose soft, lukewarm foods for the first couple of days and avoid hot, spicy, or carbonated items. Hydration is important, but avoid straws in the initial healing period.
Keep oral hygiene gentle
Continue brushing your other teeth carefully while avoiding direct disruption of the extraction site. After 24–48 hours, a mild saltwater rinse can help keep the area clean—use gentle motions and do not forceful rinse.
Attend follow-up care
If stitches were placed or if your case requires closer monitoring, please keep the scheduled follow-up appointment so we can confirm proper healing and remove sutures if needed.
If you notice persistent bleeding, increasing pain, swelling that worsens after a few days, or any unusual sensations, contact our office so we can evaluate and provide timely care.
When a tooth is removed, we look beyond the immediate procedure to plan for function, comfort, and a natural appearance. Our goal is to help patients restore chewing ability and smile aesthetics in a way that fits their needs and long-term oral health goals.
Replacement options range from removable dentures to fixed bridges and dental implants. Implants are often recommended when the objective is to closely replicate the feel and function of a natural tooth, but the right choice depends on the individual’s health, bone support, and personal preferences. We provide clear explanations of the benefits and considerations for each option so you can make an informed decision.
Our team emphasizes coordinated care: whether a restoration is completed in our office or in partnership with specialists, we focus on predictable results, careful planning, and patient comfort throughout the process.
Extractions are sometimes the healthiest path forward when a tooth cannot be saved. With careful assessment, clear communication, and modern techniques, the process can be straightforward and well-managed. We tailor each plan to the individual, prioritize comfort, and guide patients through recovery and any necessary restorative options.
If you have questions about an extraction or want to discuss possible treatment pathways, please contact us for more information.
A dental extraction is the removal of a tooth from its socket in the jaw. It is recommended when a tooth cannot be predictably restored or when it poses a risk to surrounding teeth and tissues. Common reasons include severe decay, advanced periodontal disease, extensive fractures, or problematic wisdom teeth.
Before recommending extraction, the team evaluates all conservative alternatives and explains why removal is the safest path forward for your overall oral health. We review your medical and dental history, take radiographs, and discuss how extraction fits into your longer-term treatment plan. Our goal is always to preserve natural teeth when possible and to help you understand the rationale when extraction is the best option.
Deciding whether to save or extract a tooth involves a comprehensive clinical exam, diagnostic imaging, and a review of the tooth's structural integrity and surrounding bone support. The dentist considers factors such as the extent of decay, root anatomy, presence of infection, fracture complexity, and periodontal stability. Patient health, medication use, and preferences are also important in shaping the recommendation.
When conservative treatments like root canal therapy, crowns, or periodontal therapy offer a predictable outcome, those options are prioritized. If those measures are unlikely to restore function or protect adjacent teeth, the office explains the benefits and risks of extraction and outlines subsequent restorative choices so patients can make an informed decision.
On the day of the extraction, you will receive a focused exam and any necessary imaging to confirm the treatment plan. The area will be numbed with local anesthesia and, if appropriate, additional relaxation options will be discussed to ensure comfort throughout the procedure. The clinician will describe each step before beginning and monitor you during and after the extraction until you are ready to leave.
Simple extractions typically involve loosening and removing a visible tooth and are relatively quick, while surgical extractions may require small incisions and removal of bone to access impacted or broken teeth. The practice emphasizes clear communication and safe technique to limit complications and support a smooth recovery.
Most extractions are performed under local anesthesia that numbs the specific area so patients feel little to no pain during the procedure. The dental team discusses comfort preferences and medical considerations with each patient and can offer oral or nitrous oxide sedation for additional relaxation when appropriate. In more complex cases, coordination with an oral surgeon allows for deeper sedation or general anesthesia, if indicated.
Before using any sedative, the team reviews your medical history, current medications, and any special instructions such as fasting or transportation needs. Clear preoperative guidance helps ensure safety and comfort whether you receive local anesthesia alone or combined with a sedation option.
A simple extraction is performed on a tooth that is fully visible in the mouth with straightforward root anatomy; the dentist uses instruments to loosen and remove the tooth after numbing the area. These procedures tend to be faster and have a predictable recovery profile. Patients are observed briefly after the procedure and receive instructions for managing bleeding, swelling, and pain at home.
Surgical extractions are needed when a tooth is broken at the gum line, impacted, or has complex root anatomy that cannot be accessed easily. Surgical removal may include a small incision, elevation of tissue, or removal of a bit of bone to free the tooth, and sometimes requires sutures. In complex scenarios, we refer to or collaborate with an oral and maxillofacial surgeon to ensure the safest outcome.
Initial recovery after an extraction typically takes a few days, with the first 24–72 hours being the most active period for swelling and discomfort. Mild to moderate pain that responds to recommended analgesics, some swelling, and light oozing of blood are common and usually improve each day. Most patients are able to resume normal light activities within a couple of days, though strenuous exercise should be avoided while healing progresses.
Full soft tissue healing continues over several weeks, and the underlying bone remodels over months. The office provides specific post-operative instructions—such as protecting the blood clot, maintaining gentle oral hygiene, and following diet recommendations—to help prevent complications and support uncomplicated healing. If symptoms worsen or new concerns arise, contacting the practice promptly allows for timely evaluation.
While most extractions heal without issue, potential complications include dry socket (loss of the blood clot), infection, prolonged bleeding, and numbness from nerve irritation in rare cases. Dry socket typically causes increased pain a few days after the procedure and is treated by the clinician with medicated dressings and pain management. Infection is addressed with appropriate care and, when indicated, antibiotics tailored to the clinical situation.
The dental team screens for risk factors such as tobacco use, certain medications, or systemic health issues that can increase complication risk and advises preventive steps accordingly. Any persistent or worsening symptoms should prompt immediate contact with the office so the care team can assess the situation and provide timely treatment to protect your oral health.
In the first 24–48 hours, protect the blood clot by avoiding vigorous rinsing, spitting, or using a straw, and by following the gauze instructions provided by your clinician. Gently manage swelling with intermittent ice on the face during the first day and follow medication directions for pain control. Maintain hydration and stick to soft, lukewarm foods while avoiding crunchy, spicy, or very hot items that could irritate the site.
After the first one to two days, you can begin gentle saltwater rinses to cleanse the area and support healing, taking care to rinse softly. Continue routine oral hygiene for your other teeth while avoiding direct brushing of the socket until it has begun to close. Keep scheduled follow-up visits so the team can check healing and remove sutures if needed.
Replacing a missing tooth is important for maintaining chewing function, speech, and the long-term health of surrounding teeth and bone. Replacement choices include removable options such as partial dentures, fixed bridges that span the gap using adjacent teeth for support, and dental implants that replace both the root and crown for a solution that closely mimics a natural tooth. Each option has specific advantages and considerations related to durability, maintenance, and suitability for the patient’s oral anatomy.
The practice discusses the benefits and clinical requirements of each restorative path so you can choose the solution that fits your goals and health profile. When implants are considered, imaging and bone assessment help determine timing and any need for augmentation procedures, and the team coordinates care to achieve predictable aesthetic and functional results.
Specialist referral to an oral and maxillofacial surgeon is recommended for extractions that are complex or carry higher risk, such as deeply impacted wisdom teeth, teeth with unusual root anatomy, or cases with significant infection or bone loss. Specialists have advanced training and facility resources for deeper sedation or surgical techniques that may be needed for safe removal. The primary dentist will explain when a referral is in the patient’s best interest and coordinate details of the transfer of care.
Working with specialists ensures patients receive the right level of care while preserving continuity and communication across providers. Whether the extraction is completed in our office or with a specialist, we remain involved in follow-up and in planning any subsequent restorative work to restore comfort, function, and appearance.
We recognize that dental anxiety is common and take a patient-centered approach to minimize fear and enhance comfort throughout evaluation and treatment. The team provides clear explanations of each step, discusses comfort and sedation options, and tailors the pace of care so patients feel informed and supported. Relaxation techniques, nitrous oxide, or oral sedation can be considered based on medical suitability and patient preference.
Our staff prioritizes compassionate communication and careful planning to create a calm environment from consultation through recovery. If you have concerns about anxiety, medical conditions, or past dental experiences, share them during your appointment so the team can build a plan that addresses your needs and helps you feel safe during the procedure.


