At the office of Strohman Family Dental, we focus on restoring more than just the look of your smile. Missing teeth can change the way you eat, speak, and express yourself — and they can set off a chain of dental problems if left unaddressed. This page explains how dental bridges work, when they’re a suitable choice, and what to expect before, during, and after treatment so you can make an informed decision about replacing missing teeth.
Losing a tooth isn’t only a cosmetic concern. When a gap exists, the neighboring teeth can slowly shift toward the empty space, altering your bite and making chewing less efficient. Over time, these changes can lead to increased wear on certain teeth, new areas of sensitivity, and even discomfort in the jaw joints.
Missing teeth also alter how your facial muscles and soft tissues behave. Without the normal tooth roots and biting forces, the jawbone can gradually resorb, which affects facial contours and the way dentures or restorations fit. This bone loss is one reason timely replacement matters for both function and appearance.
Speech can be affected as well. Gaps in the front or back of the mouth change how the tongue and lips form sounds, which can make certain consonants more difficult to pronounce. Finally, uneven bite forces and hard-to-clean spaces can raise the risk of tooth decay and gum disease unless a thoughtful restoration is placed.
Today’s dentistry offers a range of predictable solutions to replace missing teeth. Each approach — whether a removable partial denture, a fixed bridge, or an implant-supported restoration — has strengths that make it suitable for different clinical situations. Choosing the right option depends on the number of missing teeth, the health of surrounding teeth and bone, and your personal goals for comfort and appearance.
Dental bridges provide a fixed, non-removable way to span a gap and restore continuous biting surfaces. They can be supported by natural teeth or by implants, and they’re designed to look and function much like the teeth they replace. Because bridges are attached in the mouth, they offer stability and can help preserve proper tooth alignment.
Implant-supported restorations are the most tooth-like in function because implants emulate natural tooth roots. Where implants are not feasible or when a quicker restorative path is preferred, traditional bridges remain a time-tested solution that delivers reliable results for many patients.
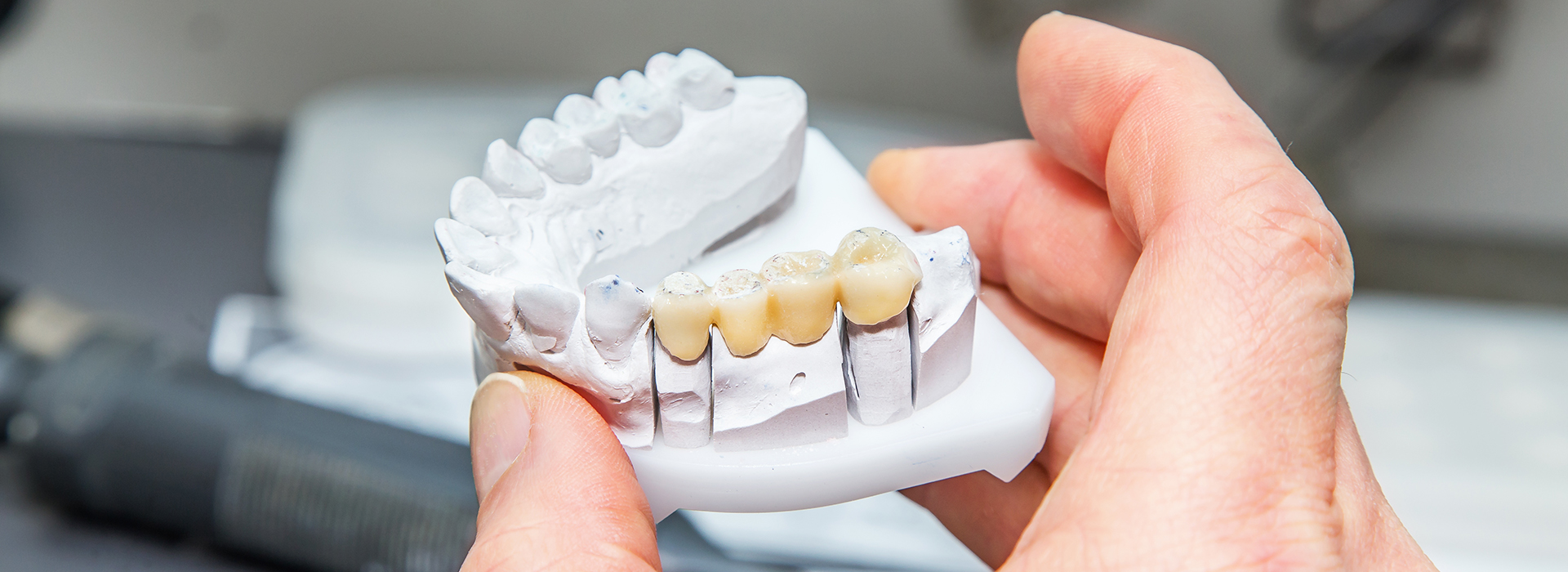
Bridges come in several common designs. A traditional fixed bridge uses crowns on the teeth adjacent to the gap (abutment teeth) to support one or more artificial teeth (pontics). This design is strong and well-suited for areas where the neighboring teeth are healthy enough to receive crowns.
A cantilever bridge is similar but anchored on only one side of the missing tooth space. It can be appropriate when there is strong tooth structure on one side and placing a crown on the opposite tooth would be undesirable. A Maryland (resin-bonded) bridge uses a metal or ceramic framework bonded to the back of nearby teeth. It’s less invasive but typically recommended for replacing front teeth where biting forces are lighter.
Implant-supported bridges replace missing teeth without altering adjacent natural teeth. Implants act like roots and support the bridge from beneath the gumline. This option preserves bone and avoids placing crowns on healthy teeth, which can be an advantage when adjacent teeth are sound and you’re seeking a long-term solution.
Effective bridge treatment begins with a comprehensive evaluation. During the initial assessment, your clinician will review your oral health, the condition of neighboring teeth, gum health, and the quality of the jawbone. Digital X-rays or 3D imaging may be used to gather precise information about the anatomy involved and to plan the restoration accurately.
If active gum disease or untreated decay is present, those conditions must be addressed before a bridge is fabricated. Healthy gums and stable supporting teeth are essential for predictable outcomes. In cases where implants are planned, bone grafting or other preparatory procedures may be recommended to create a stable foundation for long-term success.
Your personal goals and daily habits are part of the planning conversation, too. The team will discuss aesthetic preferences, expectations for maintenance, and any considerations such as grinding or clenching that might affect material choices. This collaborative approach helps ensure the selected restoration aligns with both functional needs and how you want your smile to look.
For a traditional fixed bridge, the process commonly spans multiple visits. The supporting teeth are prepared and shaped to receive crowns, impressions are taken to create a precise restoration, and a temporary bridge protects the area while the permanent piece is crafted. Before final cementation, the fit, shape, and shade are verified so the restoration feels comfortable and blends with your natural teeth.
Implant-supported bridges involve a surgical phase to place implants into the jaw. After placement, there is a healing period during which the implant integrates with bone — a biological process that can take several months. Temporary restorations can often be used during healing so you aren’t left without teeth while the implants stabilize.
After your bridge is in place, oral hygiene remains crucial. Bridges require regular cleaning beneath and around pontics to prevent plaque accumulation; special flossing tools, interdental brushes, or water flossers can help. Routine dental visits allow professionals to monitor the restoration’s fit and the health of supporting teeth and gums. With proper care and regular check-ups, bridges can provide many years of dependable service.
At our office, we approach each case with individualized planning and attention to detail so your new restoration supports both oral health and a confident smile. If you’d like to learn more about dental bridges or explore which restoration is right for you, please contact us for additional information.
A dental bridge is a fixed restoration that replaces one or more missing teeth by spanning the gap with artificial teeth called pontics. The bridge is anchored to adjacent natural teeth or dental implants, providing a stable chewing surface and restoring the continuity of your smile. Bridges are designed to blend with surrounding teeth so they look and function like natural dentition.
Beyond aesthetics, a bridge helps maintain proper bite alignment by preventing neighboring teeth from drifting into the empty space. It can improve speech and chewing efficiency that are often affected when teeth are missing. A thoughtful restoration supports overall oral health and helps preserve facial contours over time.
Common bridge designs include the traditional fixed bridge, which uses crowns on abutment teeth to support one or more pontics, and the cantilever bridge, which is anchored on only one adjacent tooth. A Maryland or resin-bonded bridge uses a bonded framework attached to the back of nearby teeth and is often used in low-stress areas such as the front teeth. Each design has specific indications depending on bite forces, tooth condition, and esthetic needs.
Implant-supported bridges replace missing teeth without altering healthy adjacent teeth by using dental implants as the support instead of crowns on natural teeth. This option preserves bone and can provide a very durable, tooth-like outcome when anatomy and overall health permit. Your clinician will recommend the best design based on the number of missing teeth and the condition of supporting structures.
Good candidates for a traditional bridge typically have healthy teeth adjacent to the gap that can be prepared to receive crowns, along with stable gum tissue and adequate bone support. If adjacent teeth are heavily restored or compromised, or if bone loss is present, an implant-supported solution may be a more appropriate choice. A thorough clinical exam and imaging, such as digital X-rays, help determine whether a bridge is the most predictable option.
Your overall health, oral hygiene habits, and any parafunctional behaviors such as heavy grinding or clenching are also considered when planning a bridge. Untreated decay or active gum disease must be managed before fabrication to reduce the risk of failure. The treatment team will review your goals, examine your mouth, and present options that align with long-term oral health and function.
An implant-supported bridge is anchored on dental implants that act like tooth roots, while a traditional bridge is supported by crowns on adjacent natural teeth. Because implants support the restoration from within the jawbone, they help preserve bone volume and avoid the need to alter healthy neighboring teeth. This difference often makes implant-supported bridges a long-term solution for patients who have sufficient bone and want to avoid modifying good teeth.
Implant treatment involves a surgical phase and a healing period for osseointegration, which can extend the overall timeline compared with a traditional bridge. Temporary restorations can usually be used during healing to maintain appearance and function. Your clinician will weigh surgical considerations, healing time, and anatomical factors when recommending either approach.
Treatment commonly begins with a comprehensive exam and preparation of the abutment teeth, which are shaped to receive crowns that will support the bridge. After tooth preparation, impressions or digital scans are taken to create a precise restoration; a temporary bridge is placed to protect the prepared teeth while the laboratory fabricates the final piece. Once the bridge is ready, the dentist verifies its fit, occlusion, and shade, making adjustments before permanent cementation.
Following placement, the team will review home care techniques and schedule follow-up visits to monitor the restoration and surrounding tissues. Regular professional cleanings and exams allow early detection of any changes in fit or health around the abutment teeth. Communication with your clinician about comfort and function helps ensure an optimal outcome.
Daily oral hygiene is essential to preserve both the bridge and the supporting teeth; clean around the pontics and beneath the restoration to remove plaque and prevent gum disease. Use floss threaders, interdental brushes, or a water flosser to reach under the pontic area and along the margins of abutment crowns. Brushing twice daily with a fluoride toothpaste and maintaining routine dental visits supports long-term success.
Avoiding habitual behaviors that place excessive stress on the bridge, such as chewing ice or using teeth as tools, reduces the risk of damage. If you have grinding or clenching habits, your dentist may recommend a nightguard to protect the restoration. Promptly report any loosening, sensitivity, or changes in bite so they can be evaluated and addressed early.
Potential complications include decay or fracture of the abutment teeth, loosening of the bridge, and gum disease around the supporting teeth if oral hygiene is inadequate. Changes in the fit of the restoration can occur over time due to tooth movement or wear, which may lead to discomfort or difficulty cleaning under the pontic. Regular monitoring and good plaque control minimize these risks and support predictable performance.
In some cases, an abutment tooth may become compromised and require further treatment such as a root canal or replacement of the restoration. If a bridge fails or the supporting teeth are lost, alternative solutions like implant-supported restorations may be explored. Your dentist will discuss potential risks based on your specific oral health and plan follow-up care to reduce complications.
Yes, bridges can replace multiple adjacent missing teeth by incorporating additional pontics between abutment crowns, provided there is adequate support from healthy abutment teeth and stable bite conditions. Long spans without implant support can place increased forces on the abutments, so clinicians carefully evaluate whether a multiunit bridge is appropriate. When several teeth are missing in a row, implant-supported bridges are often a preferred alternative because implants distribute forces to the bone.
The decision depends on the location of the missing teeth, the condition of neighboring teeth, and functional demands. A thorough assessment, including imaging, helps determine whether a traditional multiunit bridge, implant-supported restoration, or removable partial denture best meets the clinical and esthetic goals. Your dentist will explain the advantages and limitations of each option for your situation.
Common materials include porcelain fused to metal, all-ceramic systems such as zirconia, and metal frameworks for resin-bonded bridges. All-ceramic and zirconia bridges offer excellent esthetics and a lifelike translucency that closely matches natural teeth, making them a popular choice for visible areas. Porcelain fused to metal provides strong support with a durable metal substructure, which can be advantageous in areas with high biting forces.
Your clinician will consider occlusion, esthetic goals, and the position of the bridge when recommending materials. Advances in ceramic materials now allow durable restorations with excellent appearance, while metal-based options remain reliable for posterior restorations. Material selection is an important part of planning to ensure the restoration meets both functional and cosmetic expectations.
When properly designed, placed, and cared for, a dental bridge can provide dependable service for many years, though individual longevity varies with oral hygiene, bite forces, and routine maintenance. Regular professional exams and cleanings allow the dental team to monitor the health of abutment teeth, check the fit of the restoration, and address any concerns early. Maintaining excellent plaque control and following recommended protective measures helps extend the functional life of the bridge.
Follow-up schedules are individualized, but most patients continue with routine dental visits at intervals recommended by their clinician to ensure overall oral health. If you notice new sensitivity, looseness, or changes in how your bite feels, contact your dental office promptly for an evaluation. At Strohman Family Dental in Algona, our team emphasizes ongoing care to help restorations remain comfortable and effective over time.


